This article was originally published in the July 2019 edition of the Melbourne Catholic Magazine.
What matters most? During the federal election, Australians contemplated this very question as they pondered their future and cast their votes. Palliative Care Week, which was held 19 to 25 May, called for Australians to consider once again: what matters most?
I recollect vividly the moment I questioned my path in medicine. Training at some of the leading teaching hospitals prepared me for almost every medical encounter—except that of death.
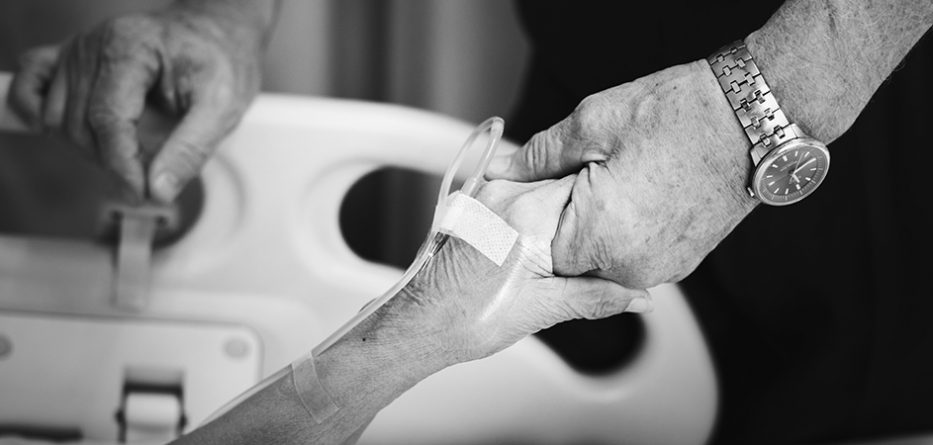
The image of an elderly man grasping tightly at my hand as his wife of more than 60 years gasped, drawing her last breaths, remains etched forever in my mind. I was 26 years old and simply did not know what to say or do or how to behave. It was the ultimate failure of my medical training.
What mattered most to him? Dignity and comfort come to mind, but he simply begged me to save his wife’s life. The default position would have been to draw up a list of investigations, autopilot into the causes of heart failure and discuss resuscitation status. This is what I did.
Today, my eyes, ears, hands and a chair are my tools. I am intrigued by the strong smell of sweet pea and hyacinth that wafts through the first room I enter. ‘From our garden,’ he informs me, ‘planted after the death of our second child.’ He recalls their first meeting at a local dance, his friends urging him on. Sixty-plus years of a happy life, not without its toils. His recollections through tears enable the unbearable to be bearable. It takes him back to a sense of wonderment of a life fully lived.
My ninth patient is a young mother. Thirty-six. Beauty and wonder are not visible in this encounter. A deep anguish is palpable, the room peppered with photographs of her young children. What matters most? They simply seek a navigator through these torrential rapids. ‘What do we say to our children?’ ‘Who pays our bills?’ ‘What do we say to schools and friends?’ These are just some of the questions I am asked.
Palliative care is deeply misunderstood. It is viewed simply as the care of the dying, without understanding the totality of what it can offer when it is done well. Stories of bad deaths arise not simply from the memory of the repugnance of death, but from one of ill preparation and a failure of professionals and society to help families delve deeply into what matters most.
The introduction of the voluntary assisted dying legislation in Victoria on 19 June reminds us of the occasional failure of medicine. Health care was designed with disease in mind, not people. The legislation introduces three major threats to health care: validating suicide as an acceptable choice; accepting substandard medical care by supporting the lack of rigour in defining eligibility; and finally, introducing into the healthcare curriculum the intentional ending of life as acceptable medical treatment. Hereby, a new generation of healthcare professionals abdicate their commitment to the sick.
Palliative care continues to encourage medicine and society to be gentler in its acceptance of death. It recognises that, for the ill, disease is a ravaging force that inexorably conquers. For the patient, the convolutions of modern medicine, the uncertainty of therapeutics, and the conundrum of multiple doctors across multiple sites bring an uncertain horizon and instil existential anguish. Their journey of illness is ultimately alienating and lonely. For many, it is the desperation for the restoration of dignity and the return of normality that drives the desire for death: ‘I want to die, let me die.’ Not: ‘Kill me.’
A request for a hastened death must be viewed as an opportunity to listen, to demonstrate concern. Patients, in my experience, respond most to authenticity. They appreciate knowing that though we see hundreds of patients, they are special in that moment. Caring and compassion are necessary for healing, but can’t be faked. Patients value not just what we say but how we are as a manifestation of our character. This authenticity must be present both in us as individuals and within our institutions and organisations.
Palliative Care Week celebrates the simple but authentic and meaningful work undertaken by many palliative care services. This goes beyond the management of pain and symptoms to include biography services, life reviews through dignity therapy, music and art therapy that form memory-making and allows for legacy-leaving, the pastoral provision of prayer, sacraments, reflections, meditations, the facilitation of family therapy sessions that allow for discourse, disclosure and closure. The efforts made to achieve the bucket list of travels, holidays, hot-air balloon rides, swims in the sea, weddings and christenings and Passover meals in a hospice or palliative care facility recognise the high human meaning and significance of giving thanks.
This legislation will pose professional and practical challenges for many people working in palliative care. It asks if our moral tradition should be reaffirmed or modified to adapt to new care-giving realities of legislation, patient demand and physician compliance. Despite such challenges, and contrary to belief, even those of us opposed to the legislation remain committed to the ongoing accompaniment of our patients. Not abandoning them. We continue to welcome all to our services. We do this because we believe the hospice approach, with its emphasis on attending to the needs of the whole person and offering support to the family, embodies the only plausible method of compassion and care to those who seek it.
This article previously appeared in The Age. It has been reprinted with permission.
Associate Professor Natasha Michael is Director of Palliative Medicine at Cabrini Health.
With thanks to Melbourne Catholic Magazine and the Archdiocese of Melbourne.